Pelvic Prolapse: A Common Cause of Pelvic Pain & Discomfort
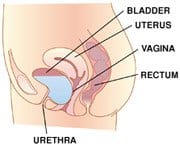
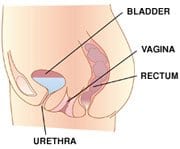
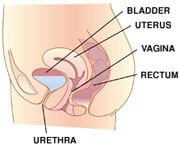
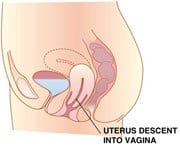
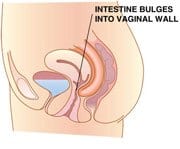
Pelvic Prolapse is caused by weakness of the pelvic tissue that then allows the organs to push down into the vagina. This protrusion causes a feeling of pressure in the vagina, lower pelvis and lower back. Depending on what is prolapsing (bladder, rectum, uterus, or intestines) symptoms can be mild or severe.
Read What Our Patients Are Saying!
"Dr. Syal is absolutely amazing. He is very down to earth and friendly. He makes you feel very comfortable and answers all your questions. He is outstanding and his staff if as well. I have been with him for a few years now after not going to ob for a WHILE... he is just the best. Hands down!"
Click here to read more reviews.
What Causes Pelvic Prolapse?
The most common cause of Pelvic Prolapse is childbirth. During childbirth, the pelvic muscles can get weak or stretched. If they don’t recover, they can’t support your pelvic organs. Other factors that can contribute to prolapse are obesity, chronic coughing, constipation, heavy lifting, smoking, and poor nutrition.
Pelvic prolapse can result in loss of urine, frequent urination, chronic constipation, back pain, and pain with intercourse. As it worsens, symptoms increase, and the bladder, cervix, or uterus may be seen coming out of the vagina. Prolapse can also occur after a hysterectomy.
How To Treat Pelvic Prolapse at home
Kegel exercises
Kegel Exercises to strengthen the muscles of the pelvis that will then better support the organs. Keegle muscles are the muscles used to stop the urine flow when urinating. With mild prolapse muscle tone may increase and prevent worsening of symptoms. Additional measures such as limiting lifting, weight loss, and eliminating smoking may help.
Emsella
is a non-invasive and revolutionary procedure that helps to strengthen the pelvic floor muscles. The Emsella treatment is delivered by relaxing in an ergonomic chair completely clothed, where electromagnetic technology penetrates the highly targeted tissue in the pelvic floor and stimulates the muscles. This strengthens the muscles and restores the support of the pelvic floor.
Pelvic Prolapse Surgical Options
For more severe cases, surgery remains a proven and effective treatment option. The type of surgery is determined by the amount and type of prolapse and the symptoms one is experiencing. Procedures are available that do not require a hysterectomy or the use of mesh. Pelvic Reconstructive Surgery is an option for treating severe pelvic prolapse. However, surgical decisions are complex and best made after an examination and discussion with your Woodlands OBGYN physician. For surgical treatments, patients will be referred to a urogynecologist.
Schedule a Pelvic Prolapse Consultation
To schedule Pelvic Prolapse consultation or to make an appointment with a specialist, please call us at 281.364.9898 or fill out an online contact form and our office will be in touch with you. Thank you for choosing Woodlands OBGYN Associates, we look forward to hearing from you!